Thoracic Spondylosis – Causes and Solutions
Manhattan Physical Therapy
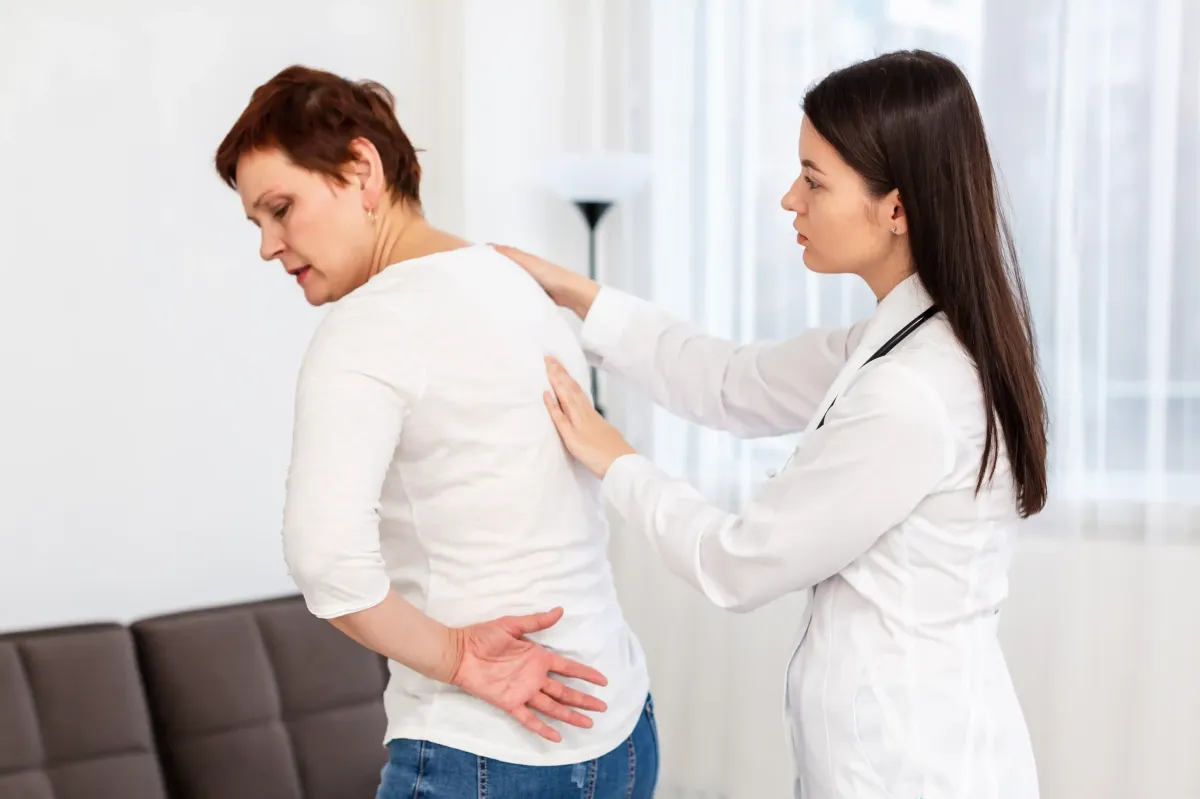
What Is Thoracic Spondylosis?
Thoracic spondylosis is a degenerative condition that affects the middle portion of your spine, known as the thoracic spine. This part of the spine runs from the base of your neck to the bottom of your rib cage and includes 12 vertebrae that connect to your ribs and help protect vital organs like the heart and lungs.
As we age, the structures that make up the spine naturally undergo wear and tear. The intervertebral discs lose moisture and elasticity, the cartilage that cushions the joints becomes thinner, and ligaments may stiffen or thicken. Over time, these changes can lead to reduced flexibility, joint irritation, and the formation of bone spurs.
Thoracic spondylosis is less common than degeneration in the neck or lower back. That’s largely because the rib cage provides extra stability and limits motion in the mid-back. Still, when degeneration does occur here, it can be uncomfortable and sometimes disruptive to daily life.
It’s also important to note that thoracic spondylosis doesn’t always develop because of a specific injury. Many people experience it gradually, simply as a result of aging and accumulated stress on the spine. In younger individuals, repetitive strain, sports-related stress, or trauma can speed up the process.
What Are the Common Symptoms?
Some people with thoracic spondylosis have no noticeable symptoms at all. When symptoms do appear, they often develop slowly and may come and go.
The most common complaints include stiffness and a dull, aching pain in the middle of the back. This discomfort often feels worse after long periods of sitting, standing, or repetitive activity, and it may improve with rest.
If degenerative changes begin to affect nearby nerves, symptoms can become more noticeable. Disc changes or bone spurs may narrow the space where spinal nerves exit, leading to nerve irritation. When this happens, pain may radiate around the chest wall or downward, sometimes mimicking rib or abdominal discomfort.
Other possible symptoms include tingling, numbness, or a sense of weakness in the arms or legs, although this is less common in thoracic conditions than in the neck or lower back. In more advanced cases, changes in posture, reduced mobility, or difficulty with balance can occur.
What Causes Thoracic Spondylosis?
Aging is the most common contributor to thoracic spondylosis. Over time, everyday stresses add up. Discs gradually dehydrate and flatten, joints experience cartilage wear, and bones may develop small spurs as the body tries to stabilize the spine.
However, aging is rarely the only factor. Prior degeneration in the neck or lower back can increase stress on the thoracic spine, making it more vulnerable over time. When one part of the spine loses normal movement or alignment, neighboring areas often compensate.
Injuries also play a role. A past fracture, whiplash-type injury, or disc injury can permanently alter spinal mechanics. Even small cracks in parts of the vertebra, such as the pars interarticularis, can set the stage for long-term degenerative changes.
Repetitive stress is another major contributor. Jobs or activities that involve frequent bending, twisting, heavy lifting, or prolonged poor posture can accelerate wear in the thoracic spine. Athletes in sports that demand repeated rotation or impact may also be at higher risk.
Bone health matters too. Conditions like osteoporosis weaken the vertebrae and increase the risk of small stress fractures, which can worsen degeneration. Genetics may influence how strong your bones and connective tissues are, making some people more prone to developing spondylosis earlier in life.
How Is Thoracic Spondylosis Diagnosed?
Diagnosis usually begins with a detailed discussion of your symptoms and medical history. If mid-back pain, stiffness, or nerve-related symptoms are affecting your daily activities or sleep, further evaluation is often needed.
A physical examination helps assess posture, spinal mobility, muscle strength, and any signs of nerve involvement. Because thoracic pain can sometimes be felt in the chest, abdomen, hips, or legs, identifying the true source isn’t always straightforward.
Imaging studies play an important role. X-rays can reveal disc space narrowing, bone spurs, changes in spinal alignment, or signs of old fractures. It’s worth noting that many adults, especially over age 60, show some degenerative changes on imaging even if they don’t have symptoms.
If nerve compression is suspected, an MRI may be recommended. MRI scans provide detailed images of discs, nerves, and soft tissues, helping identify whether degeneration is pressing on the spinal cord or nerve roots.
What Are the Treatment Options for Thoracic Spondylosis?
Treatment for thoracic spondylosis is almost always conservative at first. The main goal is to reduce pain, improve movement, and help you return to normal daily activities without making symptoms worse.
For many patients, a combination of activity modification and guided care works well. Short periods of rest can help during flare-ups, but prolonged bed rest is usually discouraged. Staying inactive for too long can lead to stiffness, muscle weakness, and slower recovery.
Pain management may include anti-inflammatory medications or short-term pain relievers prescribed by a doctor. These don’t fix the underlying degeneration, but they can make symptoms more manageable while you work on long-term solutions.
Physical therapy plays a central role. A structured program focuses on improving posture, restoring thoracic mobility, strengthening supportive muscles, and reducing stress on irritated joints and nerves. Therapy also helps correct movement patterns that may have contributed to the problem in the first place.
In certain cases, a back brace may be recommended temporarily. This can help stabilize the spine during healing after a fracture or calm symptoms during a painful phase. Bracing is usually short-term and combined with active rehabilitation.
Surgery is considered only when conservative care fails or when there is significant nerve compression, spinal instability, or progressive neurological symptoms. Procedures may involve removing pressure from nerves or stabilizing the spine, but this is reserved for more advanced cases.
Managing Thoracic Spondylosis at Home
Day-to-day habits make a real difference when managing thoracic spondylosis. Small changes, done consistently, often reduce flare-ups and slow progression.
Posture is a big one. Long hours of slouching, especially while sitting at a desk or looking down at a phone, increase strain on the mid-back. Sitting with your chest gently lifted, shoulders relaxed, and head stacked over your torso helps distribute forces more evenly.
Light activity is usually better than complete rest. Walking keeps blood flowing, supports joint health, and prevents stiffness without overloading the spine. The key is moderation and listening to your body.
Heat therapy can help relax tight muscles and ease stiffness, while ice may be useful during painful flare-ups. These are simple tools, but many people find them effective when used appropriately.
You may need to avoid heavy lifting, repetitive twisting, or prolonged bending during painful phases. Gradually reintroducing activities under professional guidance is safer than pushing through pain.
If symptoms change, worsen, or start affecting balance, strength, or breathing, it’s important to seek medical advice rather than trying to manage everything on your own.
Physical Therapy and Exercise for Thoracic Spondylosis
Exercise is one of the most effective long-term tools for managing thoracic spondylosis. When done correctly, it reduces pain, improves mobility, and helps protect the spine from further stress.
A good exercise program focuses on posture, flexibility, strength, and control. The aim is not to “push through” pain, but to restore balanced movement and support around the spine.
Thoracic Mobility and Stretching Exercises
Cat-Cow Stretch
This movement gently improves flexibility through the thoracic and lumbar spine.
Perform 10 slow repetitions in each direction, focusing on controlled breathing.
Foam Roller Thoracic Extension
This stretch helps counteract forward-rounded posture and stiffness in the mid-back.
Move slowly and stay within a comfortable range.
Thoracic Rotation Stretch
Rotation is often limited with thoracic spondylosis. Controlled rotational stretches can improve movement without excessive strain.
Strengthening Exercises for Support and Stability
Plank
Builds core strength, which reduces load on the spine. Start with short holds and gradually increase.
Bird Dog
Improves spinal stability and coordination. Focus on slow, controlled movements rather than height.
Single-Arm Dumbbell Row
Strengthens the upper and mid-back muscles that support posture and reduce stress on spinal joints.
Swimming and other low-impact activities can also be excellent options. Water reduces joint load while allowing you to move more freely. Before starting or progressing any exercise routine, it’s best to work with a physical therapist who can tailor the program to your specific condition and symptoms.
Long-Term Outlook and Practical Solutions
Thoracic spondylosis is a long-term condition, but it doesn’t have to control your life. Many people manage their symptoms successfully and stay active with the right approach.
If mid-back pain or stiffness from thoracic spondylosis is limiting your daily life, you don’t have to manage it alone. The team at Manhattan Physical Therapy can help you move better and feel more comfortable with a personalized treatment plan. Call (212)-213-3480 to schedule an appointment and get expert guidance for your recovery.
What Do They Say About Us?
Alexander Liu
"Everyone on the team at Manhattan Physical Therapy is super nice and caring. They were able to pretty quickly diagnose my knee and hip problems and immediately put me to work to reduce the pain.."
Henry Myerberg
"You're not just a patient when you come to the Manhattan Physical Therapy. You feel like family there. In particular, Erica with her colleagues John, Lidia and Joe not only fix and improve you physically, they make you feel welcomed and cared for.."
Hakyung Kim
"Everyone is so kind and helpful! my knee and hip pain have improved massively since starting Manhattan PT, highly recommend to anyone. special thanks to Bianca, Lidia, Joe, and John!"
Manhattan Physical Therapy
✆ Phone (appointments):
(212) 213-3480
Address: 385 5th Ave, Suite 503, New York, NY 10016

